Your Dermatology Skin Conditions
Atopic Dermatitis (Eczema)
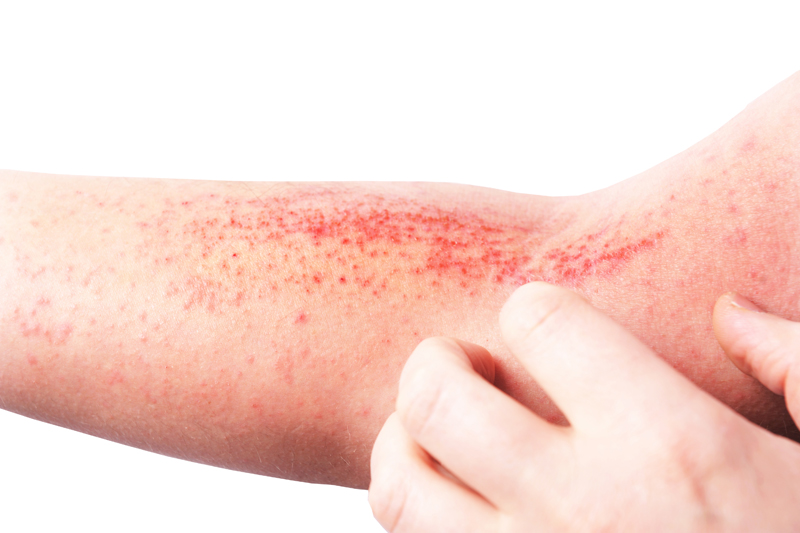
Atopic dermatitis refers to a variety of skin conditions which lead to red, itchy and flaky skin. It is speculated that allergens and biological factors play a role in this condition. The patient’s skin reacts abnormally and easily to irritants, food, and environmental allergens. The skin on the inner sides of elbows and knees is affected most commonly. Atopic dermatitis often occurs together with other allergic hypersensitivity diseases like hay fever, asthma and conjunctivitis. It often runs in families and is a chronic (lifelong) disease. Its symptoms can increase, disappear and reappear over time. Discovering the triggers of allergic reactions and learning to avoid them is the best approach for treatment. Topical treatments focus on reducing both the dryness and inflammation of the skin and include both dermatologist-recommended moisturizers and prescription strength topical corticosteroid creams. In severe cases, broad or narrow-band UV light therapy or oral medications may be used.
Acne
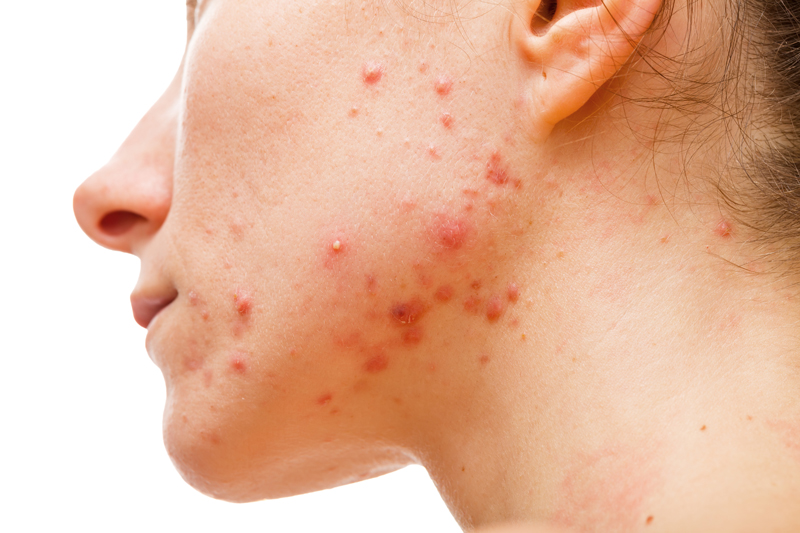
Acne is a common skin condition that affects about 70% of adolescents and a handful of adults. Areas of the skin that becomes plugged up near the oil glands form acne and most commonly affects the face, chest, shoulders and back. Acne can appear as blackheads, whiteheads, papules, pustules, and tender nodules.
During puberty acne is more common in males, but adult acne is seen more often in females. The three main causes of acne include blocked pores, male hormones and bacteria on the skin. Treatments are broad, but all aim to treat one or more of the causes of acne. These include Retin-A (tretinoin) to unplug blocked pores, antibiotics to treat the bacterial component and hormonal therapies to decrease oil production on the skin. Accutane is also an excellent and safe therapy reserved for more severe cases of cystic acne. It is important to avoid picking or scratching acne. This will trigger the acne to become inflamed and possibly cause scarring.
Psoriasis
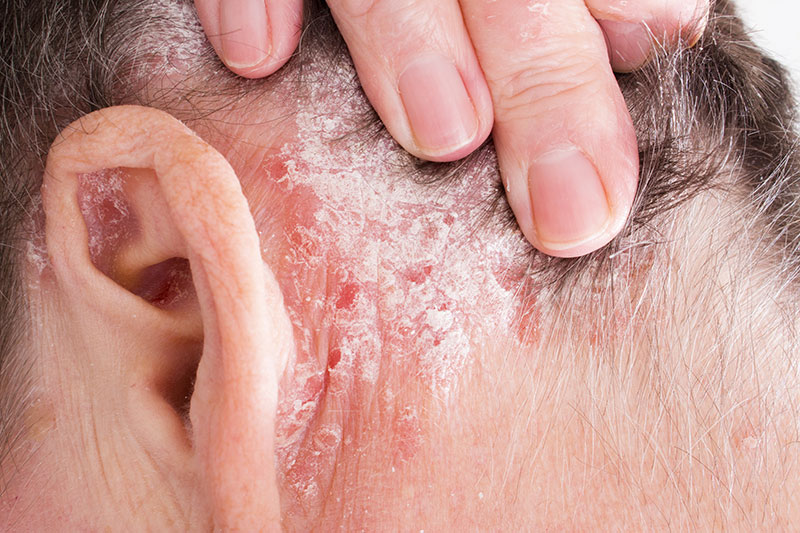
Psoriasis is a chronic skin condition that is commonly characterized by red, scaly plaques or papules that have an overlying silver scale. The lesions can occur anywhere on the body however, they are most common on the elbows, knees, scalp, buttocks, palms and soles. Men and women are equally affected and the condition affects all races. Psoriasis can present at any age, but most commonly appears between the ages of 20 and 30 or between 50 and 60. Several causes have been identified including genes and environmental factors such as bacterial infection, trauma, or drug reactions. Treatment of psoriasis can be difficult. The goal of treatment is to find the triggers and learn to avoid them. Topical treatments include topical corticosteroids, retinoids, and tacrolimus. Phototherapy and systemic therapies are also used.
Rosacea
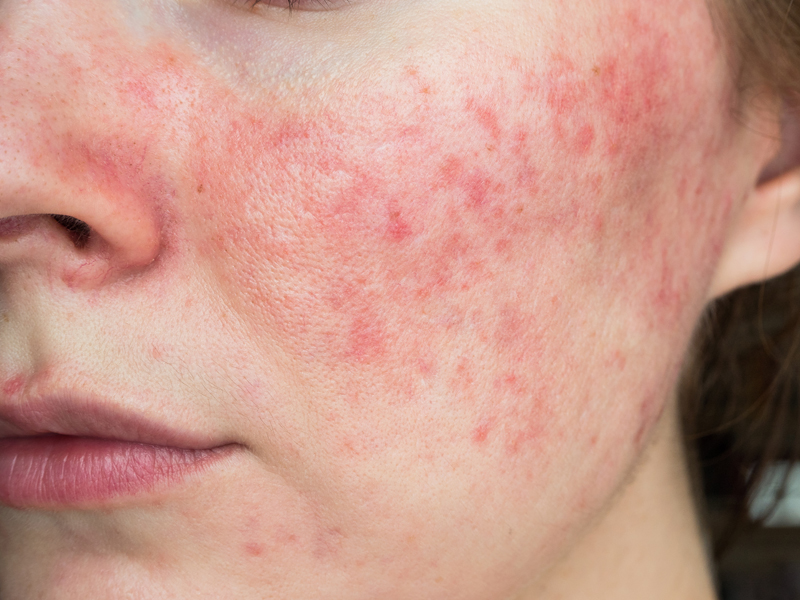
Rosacea is a common chronic inflammation of the skin that causes redness, dilation of blood vessels, and pimples on the nose, cheeks, chin and forehead. It is mostly seen with patients between 30 and 50 years. It is relatively common among individuals with fair skin, light hair and eye color, and among those who experience frequent blushing or flushing. It is a chronic disorder that can increase, disappear and reappear over time. Several triggers have been found to cause flares of rosacea including heat, sun exposure, hot drinks, spicy food and alcohol consumption. Preventing exposures to triggers helps to decrease flares. Topical treatments and systemic therapy along with our VBeam Laser which targets the small blood vessels seen in rosacea can help decrease the source of redness in the skin.
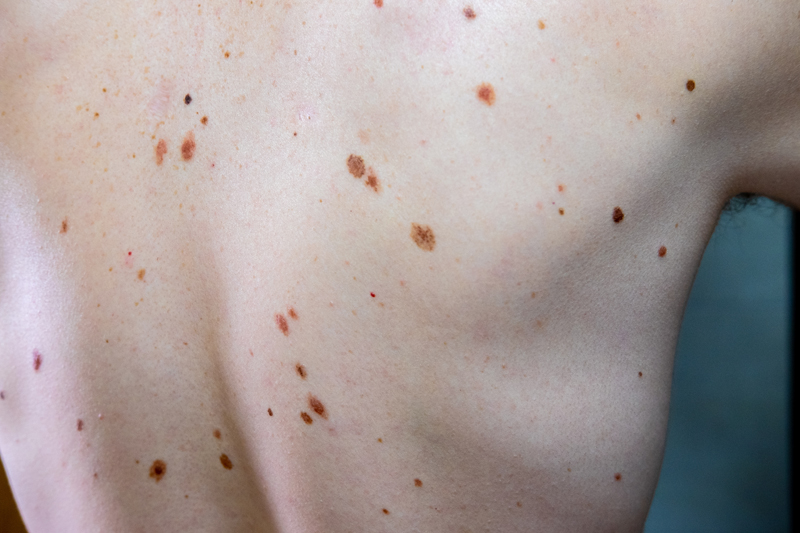
Atypical (Dysplastic) Moles (Nevi)
Atypical moles are unusual benign moles that may resemble melanoma. These moles can often appear as asymmetric, irregularly bordered, multicolored spots on the skin. With time they can increase in size. Risk factors for developing melanoma include a family history of this syndrome and one or more first or second-degree relatives with melanoma. Patients with atypical nevi who lack a family history of melanoma or the dysplastic nevus syndrome are still more likely to develop melanoma than the general population. Monthly self examination is important along with daily sun protection and professional skin exams by a dermatologist.
Melasma
Melasma is a condition characterized by tan or brown patches (hyperpigmentation) on the cheeks, nose, forehead or upper lip. Although melasma most often occurs in pregnant women due to the hormones of pregnancy, it is also seen in women with darker skin types and in those taking birth control pills or hormone replacement therapy. Sun exposure is also a strong risk factor for melasma and likely worsens the condition. There are a number of treatments available for melasma. Topical therapies such as retinoids and hydroquinone creams or pads are often tried first in addition to stringent sun protection. Laser therapies including the Intense Pulsed Light (IPL) treatment and the Deep FX fractionated CO2 laser can also be used in conjunction with topical therapies. Often, multiple treatments are needed and topical therapies are continued as maintenance therapy over time.

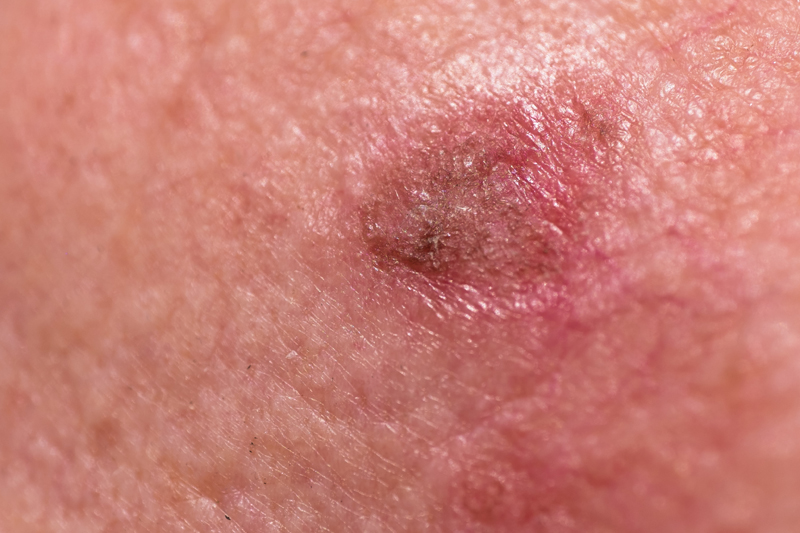
Actinic Keratoses
Actinic keratoses are red, scaly lesions found on chronically sun-exposed skin, most commonly on fair-skinned patients. They are seen frequently on the forehead, ears, nose and hands. If not treated in time, actinic keratoses gradually develop into squamous cell carcinomas. These lesions are most commonly treated with liquid nitrogen (cryosurgery) which causes the lesions to form a small blister and slough off during the week following treatment. Multiple topical treatments are also now available. Patients apply these topical agents at home over several weeks until the actinic keratosis disappears. Photodynamic therapy is another option for more widespread actinic keratosis. This therapy involves “painting” the skin with a chemical called aminolevulanic acid and allowing the skin to incubate for several hours following application. The skin is then exposed to a light source (usually Blu-U or Intense Pulsed Light/IPL) which activates the acid and targets and destroys the actinic keratoses. Peeling of the skin occurs for about a week following this treatment.
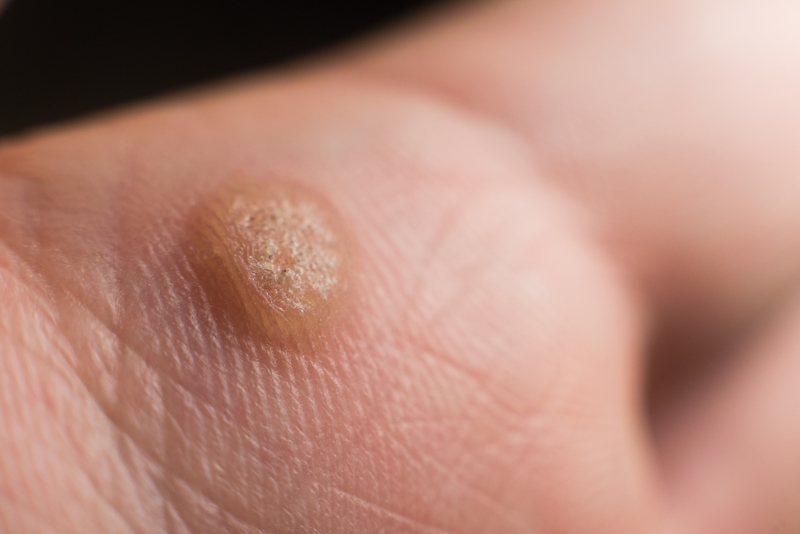
Warts (Verruca)
Warts appear as raised round growths on the skin with a rough surface. They are caused by several subtypes of the human papilloma virus and can occur in both children and adults. These lesions can be contagious, but they usually spread from one body part to another instead of from person to person. Warts can be disfiguring and embarrassing and can sometimes be painful. Several treatments are available including liquid nitrogen and electrocautery, as well as the VBeam Laser which cuts off its blood supply. More than one treatment is usually needed to successfully obliterate a wart. Multiple topical treatments are also available both over the counter and prescription strength.
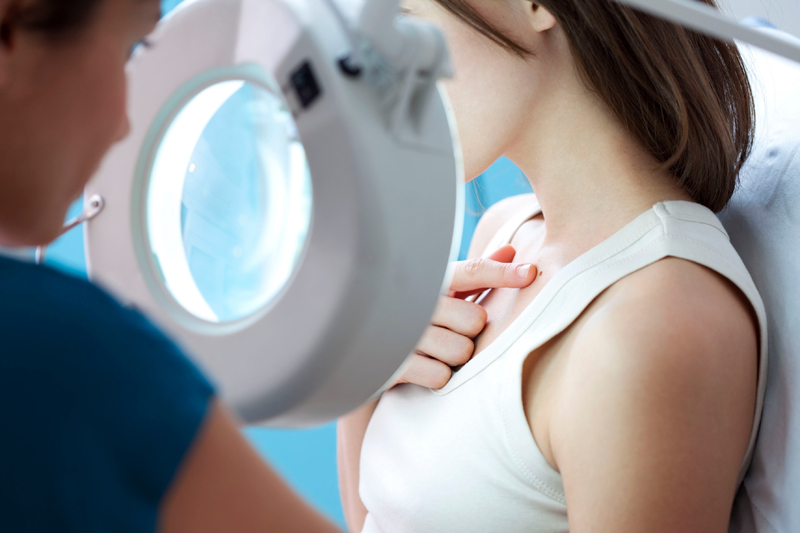
Skin Cancer Screenings
At Torrey Pines Dermatology, we recommend annual skin checks for all patients over the age of 20. Just as a patient would receive an annual physical, the skin needs to be examined every year by a dermatologist to ensure there are no suspicious growths and that hard-to-see areas are examined thoroughly. During your skin check visit, we will have a chance to address any additional concerns you may have, as well as give you up-to-date information on skin care and protection. Skin exams are almost always covered by insurance and are an important way to prevent the development of skin cancer in the future and ensure your skin is at its healthiest and best.
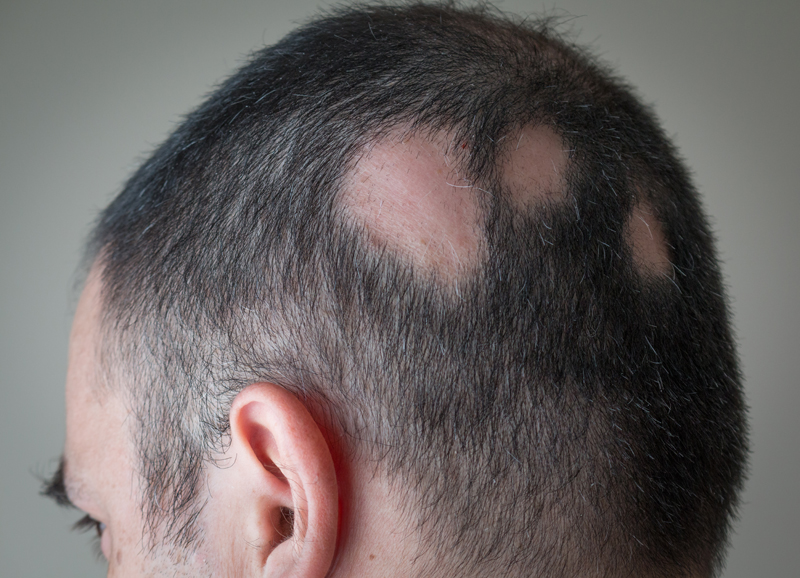
Alopecia Areata (Complete or Partial Loss of Hair)
Alopecia is a loss of hair either completely or in a patchy pattern. This condition is seen both in children and in adults and is thought to be caused by a defect in the hair follicle cycle. This cycle is in turn affected by infection, hormonal changes, stress and immune system drugs. Treatment for alopecia depends on the type of hair loss. Patchy loss of hair can be treated with multiple injections of a steroid. Other treatments include oral and topical agents. Hair transplantation can also be performed with some success.
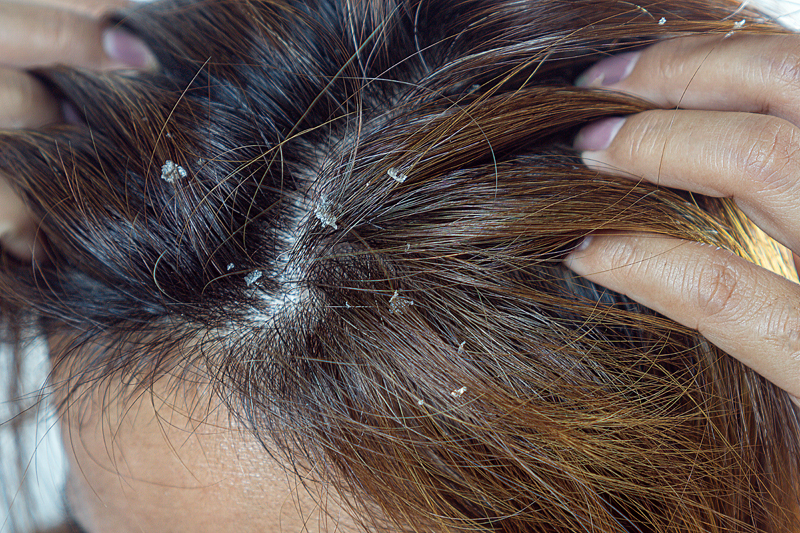
Seborrheic Dermatitis
Seborrheic dermatitis is a common, chronic inflammatory skin disorder that causes the development of flaky, white to yellowish scales on a reddish base. It usually appears in oily areas of the skin including the scalp, the eyebrows, behind the ears and sides of the nose. Cradle cap is the term used when seborrheic dermatitis affects the scalp of infants. Seborrheic dermatitis is thought to be due to a combination of excess skin oil and irritation from a yeast. Stress, fatigue, weather extremes, oily skin, infrequent hair or skin cleaning, use of lotions that contain alcohol or obesity may increase the risk. The primary form of treatment for flaking and dryness common in seborrheic dermatitis is with over-the-counter dandruff or medicated shampoos. Prescription shampoos containing ketoconazole or corticosteroids can be used in the more severe cases. A common misconception is that the scaling associated with seborrheic dermatitis is due to dryness of the scalp and that shampooing should be minimized. It is actually just the opposite. Because the yeast feeds on the oil of the scalp and causes more redness and scaling, shampooing more frequently can help to lessen the condition.
Contact Torrey Pines Dermatology & Laser Center to schedule a consultation appointment for Clinical Dermatology Services in La Jolla, CA. We look forward to hearing from you!
View Results from Actual patients
Dermatology Before & After

